The Court of Auditors' report on the future of health insurance, made public on November 29thhas been much commented on for its binding proposals for liberal doctors. But another point addressed by the "Wise Men" went unnoticed. This is the "cost of some new treatments" especially in cancer, pointed out in page 26 of the reportand the burden they may place on our health care system.
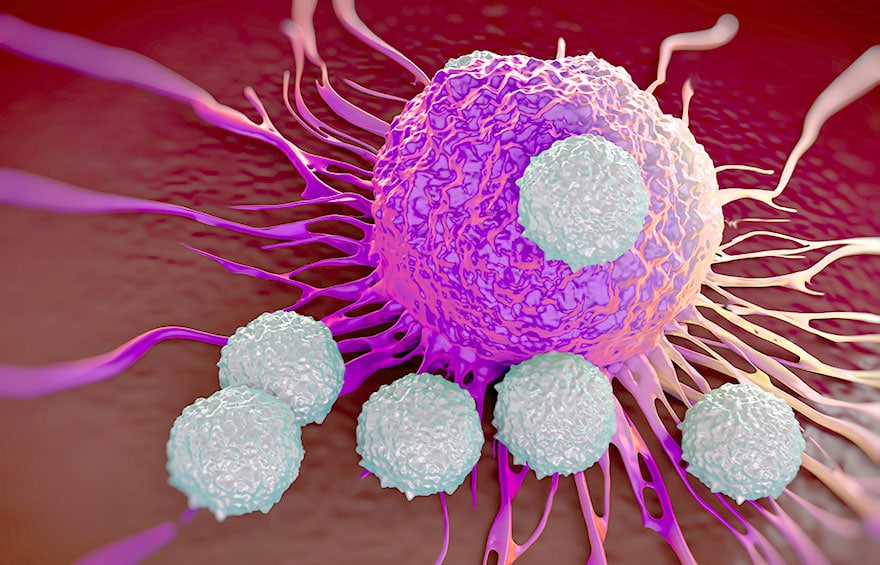
Ahe proposed gene therapies for cancer are specifically cited, referred to as an "example of expensive molecules". They involve modifying certain genes in our cells to fight the disease. They are touted as promising new treatments, and it is important to look at what they could do for patients. And how they could threaten Medicare.
Currently being evaluated in France, gene therapies in cancer are not yet available in our country. However, two of them have already been approved in the United States for use in acute leukemia. And are generating enthusiasm from the American health authority, the Food and Drug Administration (FDA).
On August 30, the agency gave the go-ahead for the marketing of Kymriah, produced by the Swiss pharmaceutical company Novartis. FDA Director Scott Gottlieb, said on that occasion This landmark decision marks the breaking of a new frontier in medical innovation with the possibility of reprogramming a patient's own cells to fight a deadly cancer.
A few weeks later, an authorization was granted for Yescarta to the Californian laboratory Gilead. This therapy was qualifiedby the same FDA director, of "another important milestone in the development of a radically new scientific paradigm for treating serious diseases".
The gene therapy craze
To understand the reasons for this crazeThe first time this happened was in the 1990s. After the first successes in human genetics and the deciphering of the genome, a new horizon opened up in medicine: gene therapy, or gene therapy.
On paper, the idea is simple. Since genetic mutations cause specific diseases, why not go directly to repair these abnormalities? A corrected version of the defective gene, a "drug gene", is then sent into the body to restore the impaired biological functions.
In practice, the path turns out to be much more tortuous than expected. Although the gene therapy industry enjoys strong institutional support for research and development, attempts to treat patients are struggling to make it through clinical trials. Kymriah is the first such therapy to be approved in the United States. Closely followed by Yescarta.
Medical and financial "promises
How could two treatments obtain this sesame that is essential for marketing one month apart? The first reason is that they are gene therapies of a new kind. They use cells from our immune system, cells from the body's immune system. T-cellss, taken from cancer patients and genetically modified in the laboratory. What's special about them? The idea here is not to repair the DNA of these cells, but to introduce additional DNA into them so that they produce a molecule that they would not have made naturally.
This molecule is called chimericbecause it is produced by artificially fusing two elements, one from mice and the other from humans. The lymphocytes thus modified known as CAR-T (for chimeric antigene response T) become capable of an immune response against the disease. In other words, they can fight cancer cells.
The second explanation for the green light obtained by these therapies in the United States: they combat cancers resistant to existing treatments; acute lymphoblastic leukaemia in children for Kymriah, and in adults for Yescarta. Until now, the significant side effects of gene therapies had been a hindrance to their development. In France, experimental therapies to treat "bubble babies", these immune-deprived childrenThe first two years of treatment were due to be stopped after leukaemia had developed in some patients. But in the case of fatal diseases and without treatment, the question of side effects only takes second place. Moreover, oncology is a field where therapeutic experimentation is very widespread and the high toxicity of treatments is largely trivialized.
A shortened evaluation procedure
Finally, both Kymriah and Yescarta have benefited from a priority review procedure, i.e. a shortened FDA review process. Under this "breakthrough therapy" regime, treatments that combat a serious, potentially fatal disease can obtain initial approval based on preliminary data. This system, which limits the financial risk associated with the hazards of market access, has largely contributed to attracting investors. Investors were all the more motivated as the potential cancer market is vast.
The question arises as to whether the preliminary results obtained with these therapies will be confirmed. This is all the more acute since several similar trials in other types of cancer had to be stopped after patients have died.
Kymriah and Yescarta therapies are part of an enthusiastic movement, both from a medical and economic point of view. The hopes but also the uncertainties they bring make them part of what the sociologist Pierre-Benoît Joly nominate a "techno-scientific promise regime.". This leads public authorities, industrialists, patients and clinicians to invest in it even before having conclusive and stabilized results.
Overpriced treatments?
The medical and scientific transformations introduced by these gene therapies are also accompanied by important economic and political transformations. Debates on this subject are crystallizing around one point: the announced prices of these treatments.
Pharmaceutical companies report a total cost per patient of $475,000 for Kymriah and $373,000 for Yescarta, not including the management of side effects. This high price level puts at risk the ability of health systems in different countries to afford these treatments for all patients. The question also arises, more broadly, for the whole of Europe. so-called "innovative" cancer treatments.
Their budgetary impact is difficult to estimate today. In France, the report of the Economic, Social and Environmental Council, published in February 2017, nevertheless indicates that all "innovative" cancer drugs could cost between 1 and 1.2 billion euros per year. In order to understand how heavy the burden would be, this amount must be compared to the EUR 15 billion that cancer currently weighs, according to the 2014 data. This illness alone accounts for 10 % of health insurance expenditure.
On the "satisfied or reimbursed" mode
In response to these concerns, Novartis is proposing to market Kymriah in a relatively new contractual arrangement: pay-for-performance. If no "improvement" is only detected after a month, indicates laboratorythen the treatment will not be charged.
This "satisfied or reimbursed" approach raises several questions. What should be considered an "improvement"? Is it a total and lasting remission? And why should the evaluation stop after one month? Some French, European and American NGOs working on access to medicines are now questioning how these criteria are defined.
At first glance, "pay-for-performance" seems a simple, and even fair, principle. But in reality it shifts the terms of price negotiation to another terrain, that of the results obtained from the treatment. And there is nothing obvious about evaluating them. For example, the clinical trial that underpinned the success of Kymriah included 63 patientswhich isn't much. Evaluation in "real life" and not in clinical trials still needs to be done.
The cost of side effects and treatment administration
Another consideration is the side effects that patients experience and the cost of their treatment. Some effects such as inflammatory reactions are already pointed out about Kymriah. In addition, there are costs for the administration of the treatment, some estimating them at between $150,000 and $200,000.
Finally, it is important to note that there are few pay-for-performance experiences around the world, including in France, have so far failed to live up to the promises they made. In Italy for example, the financial returns to the government have been minimal.
This mode of price regulation fits perfectly into the "regime of techno-scientific promises" referred to above. Indeed, this regime has its own economy, which consists in including in the calculation of "value" something that goes beyond the present and commits to the future, in this case the hope that a beginning of success calls for even greater success. In the same logic, performance-based financing is designed to convince citizens and governments that if the promise is not kept, it will cost nothing.
The new gene therapies for cancer are thus likely to have significant budgetary effects for the healthcare system, in France and elsewhere. The debate, however, should not focus solely on price levels. It must also be able to question the quality of these treatments. These discussions involve more than just health expertise agencies or central administrations. They directly concern citizens and patients.
Pierre-André Juven, Post-doctoral sociologist Cermes3, Graduate School of Social Sciences (EHESS) and Catherine BourgainGeneticist, Inserm Research Fellow, Cermes3, Graduate School of Social Sciences (EHESS)
The original text of this article was published on The Conversation.